A live look at how your baby is doing.
Nonstress testing (NST) and antepartum fetal monitoring give your care team a real-time view of your baby's heart rate, movement, and uterine activity. Quiet, noninvasive, and reassuring, usually in 15 to 30 minutes.
A simple, noninvasive look at fetal well-being.
An NST records your baby's heart rate alongside their movements and any uterine activity. A reassuring pattern, small accelerations with movement, confirms your baby is getting the oxygen they need.
-
1
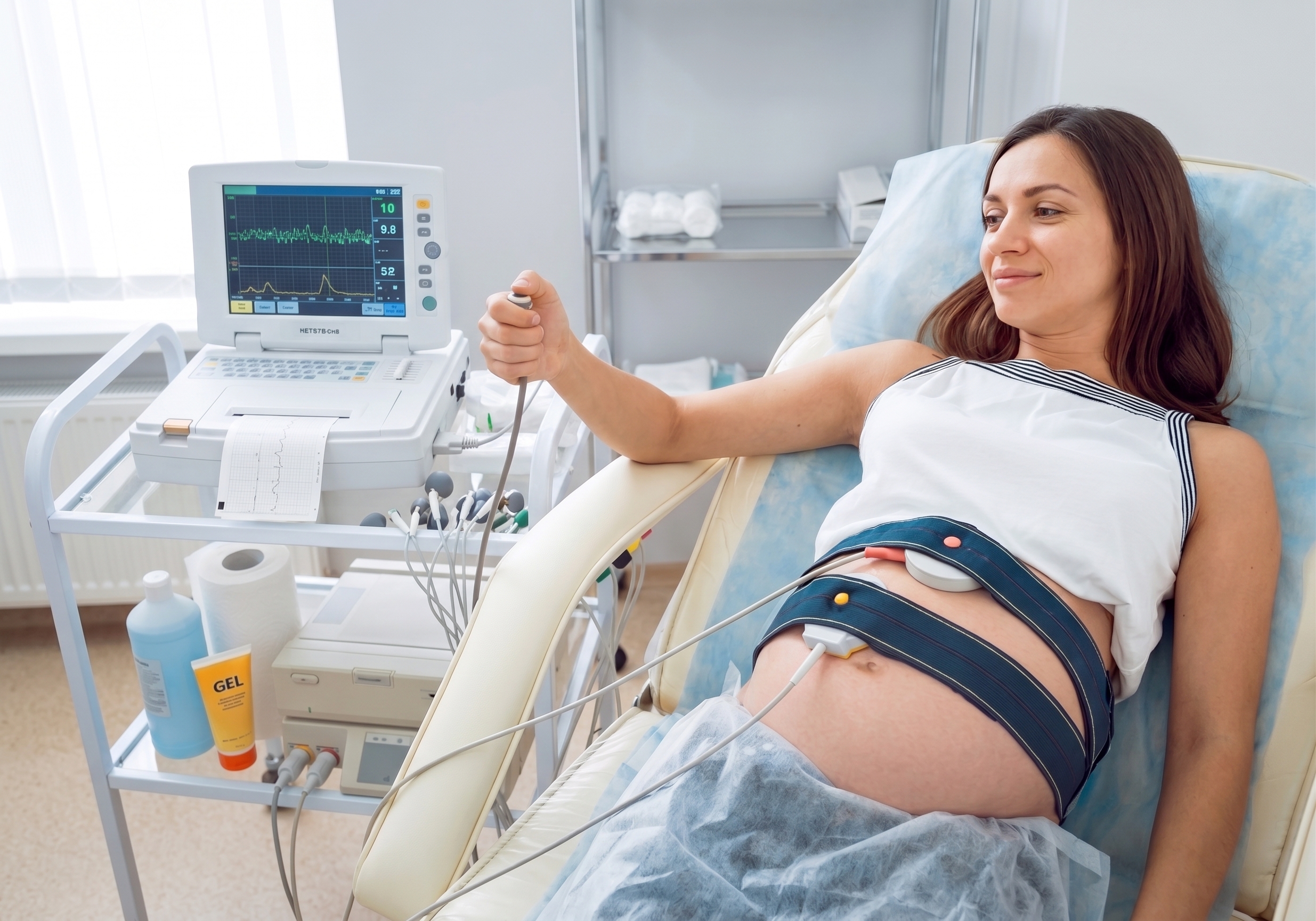
Two soft monitors are placed on your belly
One records your baby's heart rate. The second records uterine activity. Both are external, nothing invasive.
-
2
You sit comfortably for 15–30 minutes
You may be asked to press a marker each time you feel movement. No medication, no ultrasound exposure.
-
3
Results are reviewed immediately
We look for at least two accelerations with movement in 20 minutes. That's a "reactive" tracing, the goal.
-
4
Findings go straight to your OB
We communicate results the same day, with a clear next step if any is needed.
What's included in a complete picture.
Beyond the NST itself, antepartum monitoring may layer in additional tools depending on your clinical situation. Together they give a more complete read on placental function and fetal well-being.
Nonstress test
Real-time heart rate and uterine activity recording.
Amniotic fluid assessment
Ultrasound measurement of fluid volume around your baby.
Biophysical profile
Five-point ultrasound score, used when more detail is needed.
Reasons your OB may suggest closer monitoring.
Some pregnancy conditions affect how the placenta supports the baby late in pregnancy. NST testing helps confirm everything is on track, and helps catch early changes if they happen.
This is not a diagnostic tool. We'll decide together with your OB whether NST monitoring is right for your pregnancy, based on your full clinical picture.
Gestational diabetes
Higher blood sugar can change how the placenta delivers oxygen and nutrients. NST monitoring helps confirm your baby is tolerating things well between visits.
Pregestational diabetes
Long-standing diabetes carries a higher risk of placental changes and fetal growth issues. Closer surveillance gives more reassurance approaching delivery.
High blood pressure / preeclampsia risk
Elevated maternal blood pressure can reduce blood flow through the placenta. NSTs help us catch early changes before they become a problem.
Decreased fetal movement
When you notice fewer kicks, an NST gives an immediate, real-time look at how your baby is doing, usually within minutes.
Fetal growth restriction
A baby who's measuring small may be working harder to get what they need. NSTs and Doppler studies help time delivery safely.
Post-term pregnancy
After 41 weeks, the placenta gradually becomes less efficient. NSTs reassure us your baby is still tolerating pregnancy well.
Multiple gestation
Twins and higher-order multiples need closer monitoring of each baby's heart rate and growth.
Advanced maternal age
Pregnancies after 35 carry a slightly higher risk of placental issues. NSTs add a layer of reassurance late in pregnancy.
Cholestasis of pregnancy
Elevated bile acids can increase risk to the baby. NST monitoring guides timing of delivery.
Autoimmune conditions
Conditions like lupus or antiphospholipid syndrome can affect placental function. Monitoring helps protect both you and your baby.
Kidney or cardiac disease
Maternal organ stress can change how well the placenta supports your baby. NSTs add reassurance between specialist visits.
Prior pregnancy complications
A previous stillbirth, growth restriction, or preeclampsia raises the chance of recurrence. Earlier and more frequent NSTs are protective.
Medication exposures requiring monitoring
Some medications change fetal heart rate patterns. We monitor to make sure your baby is responding normally.
Subspecialty monitoring, integrated with your existing care.
NST testing at Advanced Perinatology lives alongside your ultrasound evaluations and consultation visits. Your OB stays informed at every step.
Subspecialty setting
Testing performed in a maternal-fetal medicine office.
Reviewed immediately
Results read in the room, before you leave.
Direct to your OB
Findings communicated to your provider the same day.
Recommended intervals
A clear schedule for follow-up testing if needed.
Coordinated next steps
If more evaluation is needed, we arrange it from here.

If your OB recommends fetal monitoring, we can help coordinate it.
Ultrasound, consultation, and NST testing in one place, so your third-trimester care stays simple and connected.
Talk to our team